Is Gum Disease Reversible Understanding Treatment Outcomes
Is Gum Disease Reversible? Separating Fact from Fiction in Periodontal Treatment Outcomes
The moment a dentist mentions "gum disease," it’s normal to feel a sudden drop in your stomach. Perhaps you’ve noticed a bit of blood when brushing, or maybe a tooth feels slightly different than it used to. The immediate questions that race through your mind are usually driven by fear: "Is this permanent?" and "Can I fix this?"
The internet is flooded with conflicting advice, home remedies, and frightening statistics. However, the answer to whether gum disease is reversible isn't a simple yes or no—it depends entirely on where you are in the disease's progression. Understanding this distinction is vital, as falling for common myths and misconceptions surrounding gum disease can lead to delays in treatment that allow the condition to worsen.
The Two Faces of Gum Disease: Reversible vs. Manageable
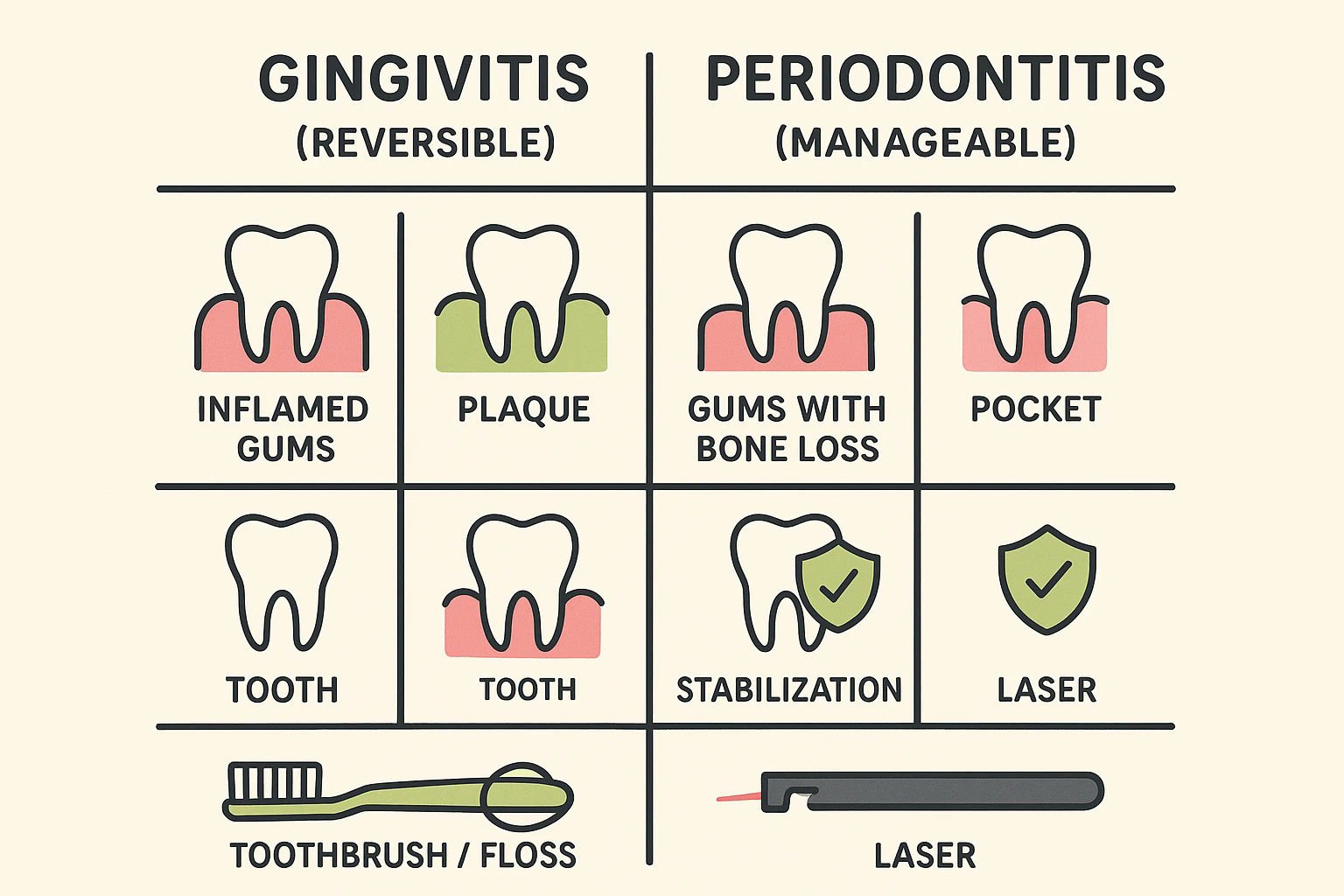
To take control of your oral health, you need to understand that "gum disease" is an umbrella term covering two very different stages of infection. The treatment outcomes for these stages differ significantly.
Gingivitis: The Warning Sign You Can Reverse
Gingivitis is the earliest stage of gum disease. It is caused by plaque buildup irritating the gums, leading to inflammation. At this stage, the connection between the tooth and the bone is still intact.
Because the underlying bone structure hasn't been damaged yet, gingivitis is entirely reversible. With professional cleaning and improved home care, the gums can return to a completely healthy, pink, and firm state. Recognizing the difference between normal gums vs gingivitis is your first line of defense; if your gums bleed when you floss, that is your body’s alarm bell ringing.
Periodontitis: The Condition You Can Halt
If gingivitis is left untreated, it advances to periodontitis. This is where the narrative shifts from "reversing" to "managing" and "halting." In periodontitis, the infection spreads below the gum line, attacking the ligaments and bone that hold your teeth in place.
Here is the hard truth: Bone that is lost usually does not grow back on its own. In this sense, the structural damage of periodontitis is often considered irreversible.
However, this does not mean the situation is hopeless. Far from it. While you may not be able to magically regrow all lost bone, modern dentistry allows us to halt the progression of the disease completely. Think of it like a house with a settling foundation. You might not be able to lift the house back to its original height instantly, but you can reinforce the foundation to ensure it never sinks another millimeter, making the structure safe, stable, and secure for a lifetime.
A Stage-by-Stage Guide to Taking Control
Understanding where you stand on the spectrum of gum disease helps remove the fear of the unknown.
1. Early Periodontitis
At this stage, slight bone loss has occurred. Pocket depths (the space between the tooth and gum) measure between 3-4mm. You might not feel pain, but the damage has begun. The goal here is to stop the infection before it compromises the tooth’s stability.
2. Moderate Periodontitis
As the disease progresses to moderate periodontitis (often classified as Stage 2 or 3), pocket depths increase to 5-7mm. The bacteria are now deep enough that toothbrushes and floss cannot reach them. Patients often wonder, can you catch gum disease from family members at this stage? While the bacteria are transmissible, the susceptibility depends on the individual's immune system and oral environment.
3. Advanced Periodontitis
In advanced stages, significant bone loss leads to loose teeth and potential shifting. Historically, this was the point where teeth were extracted. Today, however, advanced treatments can often save these teeth by eliminating the bacterial infection and reducing the pocket depths to a maintainable level.
Halting Advanced Disease: Modern Periodontal Therapies
The fatalistic view that "gum disease means losing your teeth" is outdated. At the Behrens Dental Practice, the approach to halting periodontal disease is rooted in precision and advanced technology.
The Role of Bacteria and DNA Analysis
One of the reasons traditional treatments sometimes fail is that they treat the symptoms (tartar and pockets) without identifying the specific culprit. Behrens Dental distinguishes itself by performing a microbiological DNA analysis along with staging and grading.
By identifying exactly which bacteria are causing the infection, the periodontal experts can tailor the treatment plan. It’s not just about "cleaning teeth"; it’s about targeting the specific pathogens destroying your oral health.
The Laser Revolution: Duo-Lase™
Traditional surgery often involves cutting gum tissue to access and clean the roots—a procedure that can be painful and requires significant recovery time. This is where Duo-Lase therapy changes the game.
Duo-Lase™ utilizes a dual-laser approach to treat gum disease non-invasively:
Elimination: The first laser wavelength targets and vaporizes the harmful bacteria and diseased tissue inside the gum pocket without harming the healthy tissue.
Regeneration: The second wavelength stimulates the body's own healing response (Bio-Stimulation), encouraging collagen production and helping the gum tissue reattach to the tooth.
This method effectively halts the disease progression, reduces pocket depth, and in some cases, can even stimulate a degree of tissue regeneration that was previously thought impossible without grafting.
Your 4-Step Plan to Protect Your Smile
If you are concerned about your gum health, clarity is your best ally. Here is a path forward:
Detailed Diagnostics: Don't settle for a quick look. Ensure your dental team performs a full periodontal chart and, ideally, a microbiological test to understand the bacterial load.
Targeted Treatment: Based on the specific bacteria and disease stage, a plan involving laser therapy (like Duo-Lase™) or deep cleaning can be created to stop the infection.
Home Maintenance: Once the disease is halted, your home care routine becomes the "security guard" keeping the bacteria away.
Regular Recall: Periodontitis is a chronic condition, much like diabetes. It requires monitoring. Regular visits ensure that what is gum disease essentially becomes a dormant part of your history, rather than an active threat to your future.
Frequently Asked Questions
Q: Can gum pockets shrink back to normal?
A: Yes. When the infection is removed and inflammation subsides, the gum tissue tightens around the tooth. While the bone doesn't regrow significantly, the reduction in inflammation reduces the pocket depth, making it easier to keep clean.
Q: Is laser treatment painful?
A: One of the primary benefits of Duo-Lase™ is patient comfort. Because it is minimally invasive and requires no cutting or sutures, patients typically experience far less discomfort compared to traditional gum surgery.
Q: If I have bone loss, will my teeth fall out?
A: Not necessarily. Even teeth with reduced bone support can function for decades if the gum disease is halted and the remaining support system is kept healthy and stable.
Taking the Next Step
The realization that you have gum disease can be daunting, but it is not a final verdict on your smile. Whether you are at the reversible stage of gingivitis or need to manage periodontitis, the technology and expertise exist to help you keep your natural teeth.
By combining precise diagnostics with innovative laser protocols, the team at Behrens Dental Practice transforms what was once a painful, surgical ordeal into a manageable, health-affirming journey. The first step isn't surgery—it's understanding.