How Smoking Speeds Up Gum Disease Through Biology
How Smoking Accelerates Periodontal Disease: The Biological Mechanisms
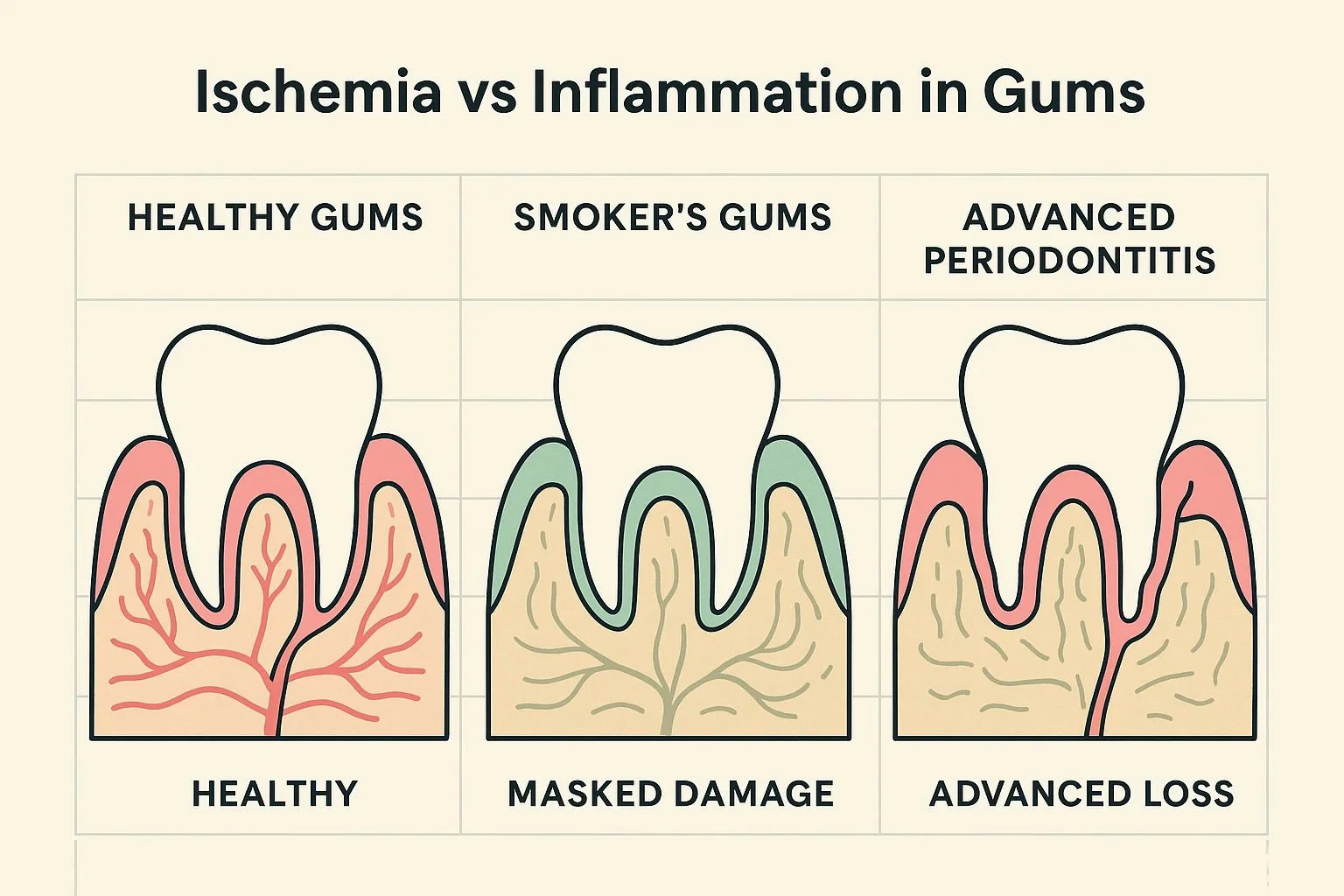
Imagine looking in the mirror, inspecting your gums, and seeing what appears to be perfectly healthy, firm, pale pink tissue. You brush and floss diligently, and you rarely—if ever—see a single drop of blood. You might understandably think your oral health is in perfect condition. But if you are a smoker, that lack of bleeding might not be a sign of health at all. In fact, it could be the ultimate biological disguise.
When we talk about the effects of smoking on oral health, most resources simply repeat the familiar warning: smoking causes what is gum disease. But they rarely explain why. Why do smokers progress through the stages of disease faster than non-smokers? And why do their gums almost never bleed, even when severe infection and bone loss are actively occurring beneath the surface?
The answer lies in nicotine's profound ability to alter your body's cellular functions. It acts like an "invisibility cloak" for infection. By the time a smoker notices their teeth feeling loose, shifting out of place, or experiencing severe bad breath, the disease has often reached advanced stages.
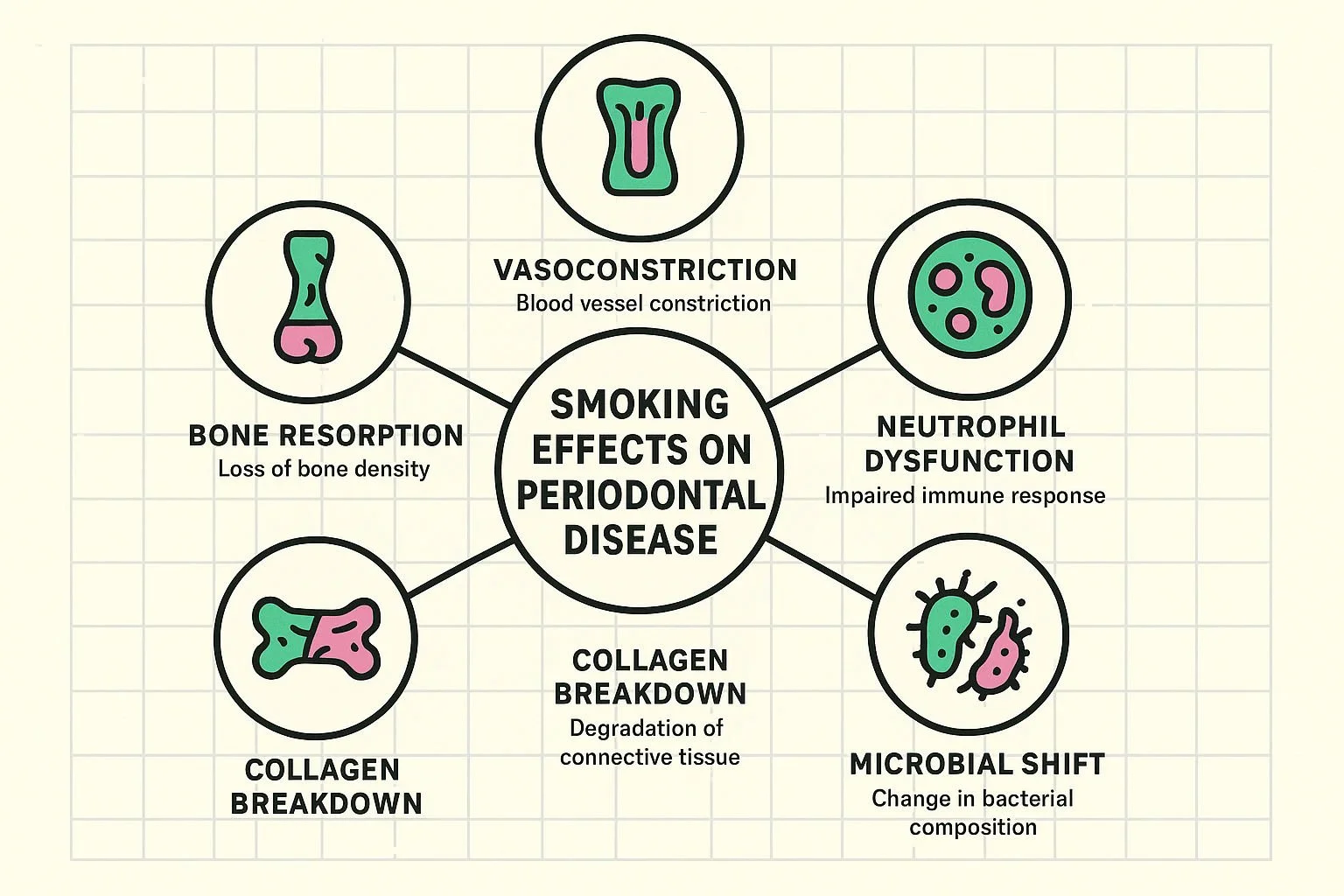
The 5-Point Biological Collapse: What Happens Beneath the Surface
To truly understand how smoking affects your gums, we need to look beyond the surface and explore the five specific biological pathways that break down when exposed to tobacco smoke.
1. Vascular Starvation (Vasoconstriction)
The most deceptive aspect of smoking and gum health is the "Vascular Lie." Nicotine is a powerful vasoconstrictor, meaning it physically shrinks your blood vessels. When an infection occurs in a non-smoker's mouth, blood rushes to the area to deliver immune cells, causing the gums to swell, turn red, and bleed easily. This inflammation is a crucial warning system.
In a smoker, the blood vessels are so constricted that nutrients and immune cells cannot easily reach the site of the infection. The pale, firm gums you see aren't healthy—they are suffering from ischemia (cellular starvation). Because the blood supply is restricted, the gums don't bleed, masking the early warning signs of disease.
2. The Failed Sentinels (Neutrophil Dysfunction)
Neutrophils are the white blood cells acting as your body’s first responders to bacterial invaders. Interestingly, smokers actually have more neutrophils in their bloodstream than non-smokers. However, exposure to tobacco smoke effectively paralyzes them. While these immune cells are present, their function is severely suppressed. They lose their ability to navigate accurately toward the bacteria and are far less capable of destroying the pathogens once they arrive.
3. The Microbial Coup (Elevated Pathogenic Bacterial Loads)
Your mouth is home to a delicate balance of bacteria. Smoking completely disrupts this ecosystem. Tobacco smoke reduces the oxygen levels within the periodontal pockets (the spaces between your teeth and gums). This low-oxygen environment is the perfect breeding ground for highly aggressive, anaerobic bacteria, such as Porphyromonas gingivalis. As these harmful bacteria multiply rapidly, they overwhelm the already compromised immune system.
4. The Structural Collapse (Impaired Collagen Synthesis)
Healthy gums tightly grip the teeth thanks to a strong network of collagen fibers. Smoking triggers an overproduction of enzymes called Matrix Metalloproteinases (MMPs). In a healthy body, MMPs help remodel tissue. But in a smoker's mouth, these enzymes go into overdrive, essentially "eating" the collagen fibers much faster than the body can rebuild them. This structural collapse causes the gums to detach from the teeth, deepening the periodontal pockets.
5. The Bone Melt (Disrupted Bone Metabolism)
Perhaps the most severe consequence of smoking is its direct impact on the jawbone supporting your teeth. Nicotine suppresses the activity of osteoblasts (the cells responsible for building new bone) while simultaneously fueling the activity of osteoclasts (the cells that break down bone tissue). This imbalance leads to rapid bone resorption. Because the process is largely painless and the typical signs of inflammation are masked, smokers often present with significantly more advanced bone loss at their initial diagnosis.
The Diagnostic Challenge: Seeing Through the Smoker's Mask
Because smoking hides the classic signs of gum disease, standard visual dental check-ups can easily miss the true severity of the problem. A quick glance might suggest everything is fine while profound destruction occurs beneath the gumline.
This is why a comprehensive diagnostic approach is absolutely critical. At The Behrens Dental Practice in London, periodontal experts utilize Micro Perio Analysis to see what the naked eye cannot. This involves a microbiological DNA test to identify the exact strains of bacteria causing the disease. By combining this precise bacterial mapping with careful staging and grading of the disease, experts can create a highly personalized treatment plan that addresses the root cause of the infection, rather than just treating the visible symptoms.
Why Traditional Surgery Struggles in Smokers
When stage 4 periodontal disease is diagnosed, standard protocols often involve surgical interventions where the gums are cut, folded back to clean the roots, and sutured. However, these traditional methods present a massive challenge for smokers.
Because the gum tissue in a smoker is already vascularly starved, cutting into it further disrupts an already fragile blood supply. The body simply lacks the biological resources—oxygen, nutrients, and functioning collagen—to heal the surgical wounds effectively. This frequently leads to painful recoveries, tissue shrinkage, and less predictable long-term outcomes.
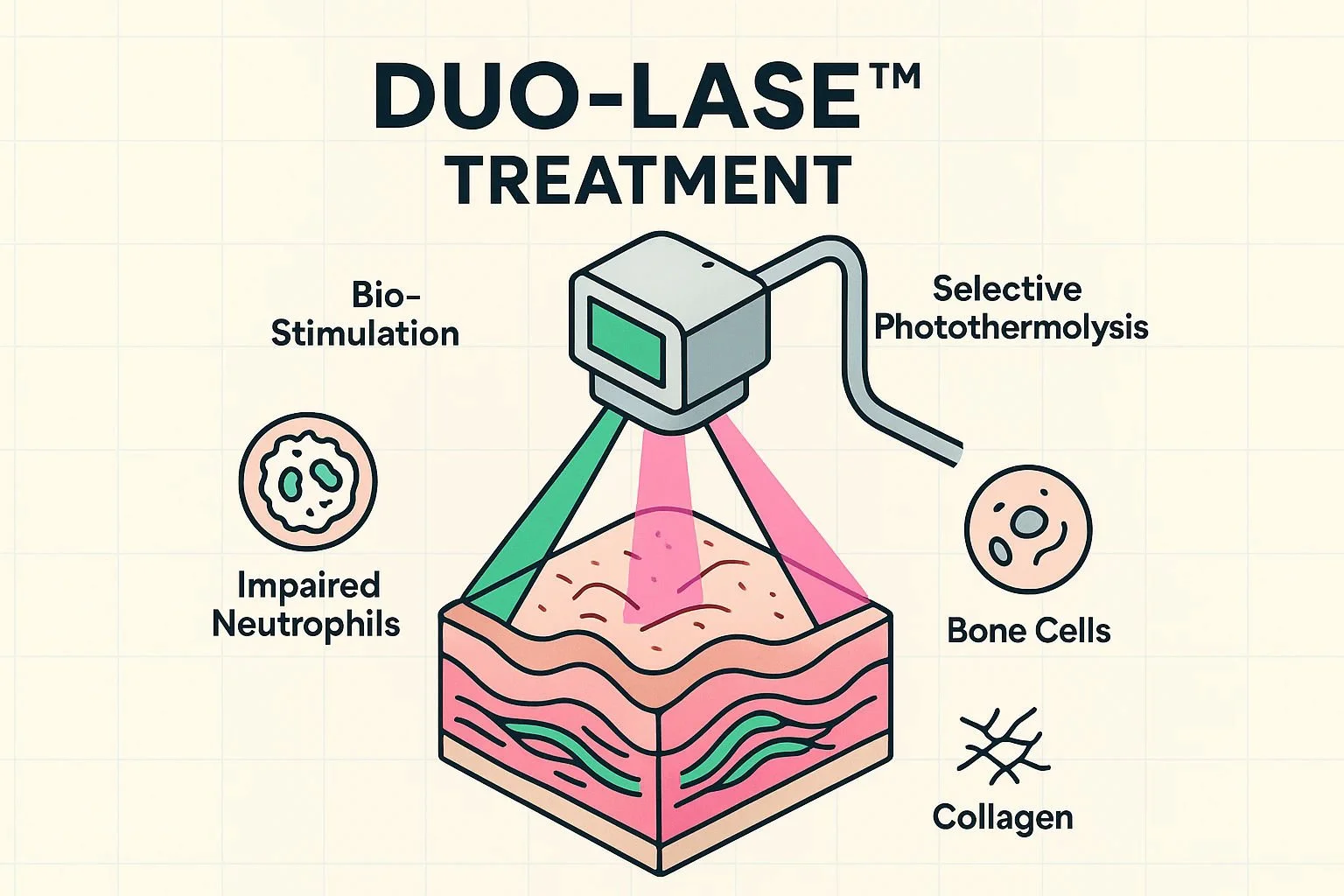
The Bio-Logic of Treatment: Introducing Duo-Lase™
If a patient's natural healing capacity is compromised by smoking, the logical solution isn't to cut away tissue, but to help the body repair itself at a cellular level. This is the philosophy behind duolase.
Duo-Lase™ is an innovative, non-invasive therapy that uses a dual-laser approach to target the disease without relying on surgical tissue manipulation. By working with the body rather than against it, this treatment is ideal for environments where healing is impaired. The process relies on "photodynamic pocket decontamination" utilizing two distinct lasers:
The Nd:YAG Laser:
This first laser specifically targets and removes the dark-pigmented bacteria that cause the disease, leaving healthy tissue unharmed. Simultaneously, it acts as a powerful anti-inflammatory for the gum tissue, actively helping it heal. Critically, the Nd:YAG laser supports the creation of a new cell layer on the root surface—including cementoblasts, which are the specialized cells that help close the periodontal pockets and reattach the gum to the tooth.
The Diode Laser:
The second laser focuses purely on bio-stimulation. It essentially "wakes up" the localized healing response, promoting cellular activity and vital collagen production in both the underlying bone and the gum tissue. Furthermore, the laser helps create a natural fibrin seal that protects the clean periodontal pocket from new bacteria while it heals.
Because Duo-Lase™ does not involve cutting or suturing, patients require an average of 10 laser sessions (which can be completed up to 3 times per week). The treatment is so gentle that it is usually performed completely without anaesthetic, and there is zero downtime afterward, offering a genuinely fast healing periodontal care experience.
The Recovery Path: Next Steps for Smokers
Realizing the hidden damage smoking causes to your gums can be a startling "aha moment," but it is also the first step toward reclaiming your oral health. The path forward involves a two-pronged approach:
Address the Environment: Reducing or quitting smoking is the single most powerful step you can take to restore normal blood flow, reactivate your immune sentinels, and allow your body to rebuild collagen.
Seek Bio-Logical Treatment: Instead of waiting for symptoms like loose teeth to appear, seek out advanced diagnostics that include microbiological testing. Once the exact bacteria are identified, a bio-stimulatory approach like Duo-Lase™ can gently remove the infection and coax your body back into a healing state. Following treatment, ongoing hygienist visits and excellent home care ensure your mouth remains healthy for years to come.
Frequently Asked Questions (FAQ)
Why don't my gums bleed even though they look receded?
Nicotine acts as a vasoconstrictor, meaning it shrinks the blood vessels in your gums. This restricts blood flow to the area. Without adequate blood flow, the gums cannot produce the redness, swelling, and bleeding that normally signal an active infection. This creates a "mask" that hides the disease while bone loss continues underneath.
Does smoking directly cause jawbone loss?
Yes. Smoking disrupts normal bone metabolism. Nicotine suppresses the cells that build new bone (osteoblasts) and stimulates the cells that break down bone (osteoclasts). Over time, this imbalance causes the jawbone supporting your teeth to literally melt away.
Why is traditional gum surgery harder for smokers to recover from?
Traditional surgery involves cutting the gums and using sutures. Because a smoker's gums have a severely restricted blood supply and impaired collagen production, the body struggles to heal the surgical wounds. This can lead to painful, slow recoveries and less successful outcomes compared to non-surgical laser therapies.
What is bio-stimulation, and why is it important for smokers?
Bio-stimulation involves using specific light energy (like a diode laser) to trigger cellular activity without generating destructive heat or requiring cuts. For smokers, whose natural healing processes are suppressed, bio-stimulation is crucial because it actively promotes collagen production and helps "wake up" the body's natural repair mechanisms at a molecular level.
Does Duo-Lase treatment hurt?
No. Because Duo-Lase™ is a non-invasive treatment that does not involve cutting or suturing the gums, it is incredibly gentle. In fact, the procedure is usually performed entirely without the need for anaesthetic, and patients experience no downtime afterward.