Why Smoking Hides Early Signs of Gum Disease
Why Smoking Masks Early Gum Disease Symptoms (And Why That's Dangerous)
If you are a smoker who brushes regularly, looks in the mirror, and sees pale, non-bleeding gums, you might assume your oral health is perfectly fine. After all, isn't bleeding the universal warning sign of gum disease?
This widespread assumption creates what dental professionals call the "Healthy Smoker Paradox." It is a dangerous misconception that leads thousands of people to search online for answers to confusing scenarios, like having no bleeding but gum disease, or gum disease without symptoms.
The unsettling truth is that your gums might be crying out for help, but smoking has simply silenced the alarm. Let's explore exactly how tobacco conceals active inflammation beneath seemingly healthy-looking gums, and why seeing through this smoke screen is the first step to saving your smile.
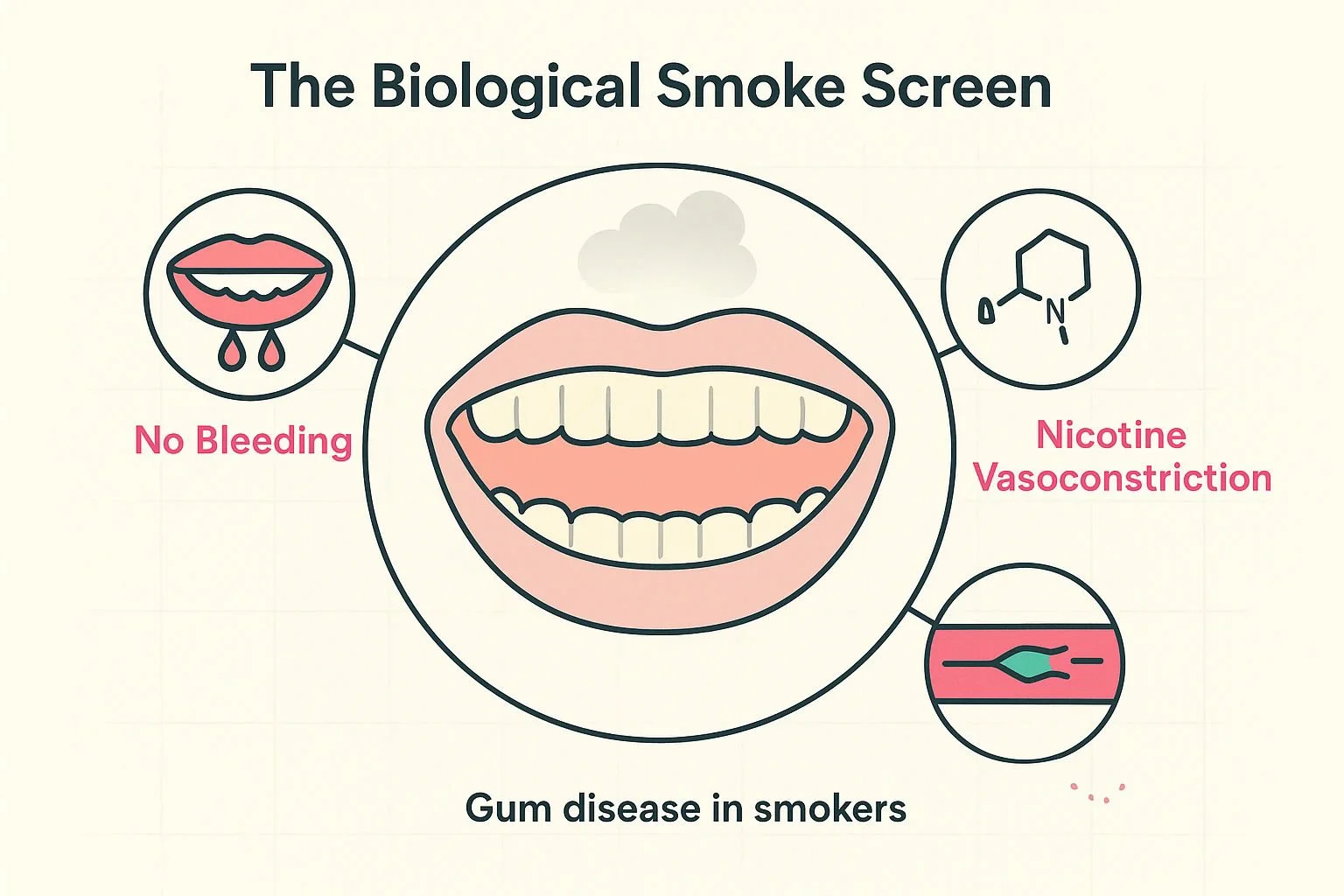
This visual explains how nicotine causes blood vessel constriction, hiding early gum disease signs like bleeding, creating a dangerous 'smoke screen' effect.
The Biological Smoke Screen: How Nicotine Hides the Alarm
To understand why smokers rarely see blood in the sink, we have to look at how nicotine interacts with the human body.
Nicotine is a powerful vasoconstrictor. This means it causes your blood vessels to shrink and narrow, dramatically reducing blood flow to your extremities—including your gum tissue.
Think of bleeding gums as the mouth’s biological smoke alarm. When harmful bacteria gather around your teeth, your body naturally rushes blood and immune cells to the area to fight the infection. This surge of blood causes swelling, redness, and the bleeding you typically see when brushing or flossing.
Nicotine essentially removes the batteries from that alarm. Because the blood vessels are physically constricted, the blood cannot rush to the surface. The fire (bacterial infection) is still spreading, but the warning sirens have been shut off.
This leads to a condition known as gingival fibrosis. Instead of looking angry and red, a smoker's gums often look pale, overly firm, and tightly bound. They might look "too white," which is actually a sign of poor circulation, not exceptional health.
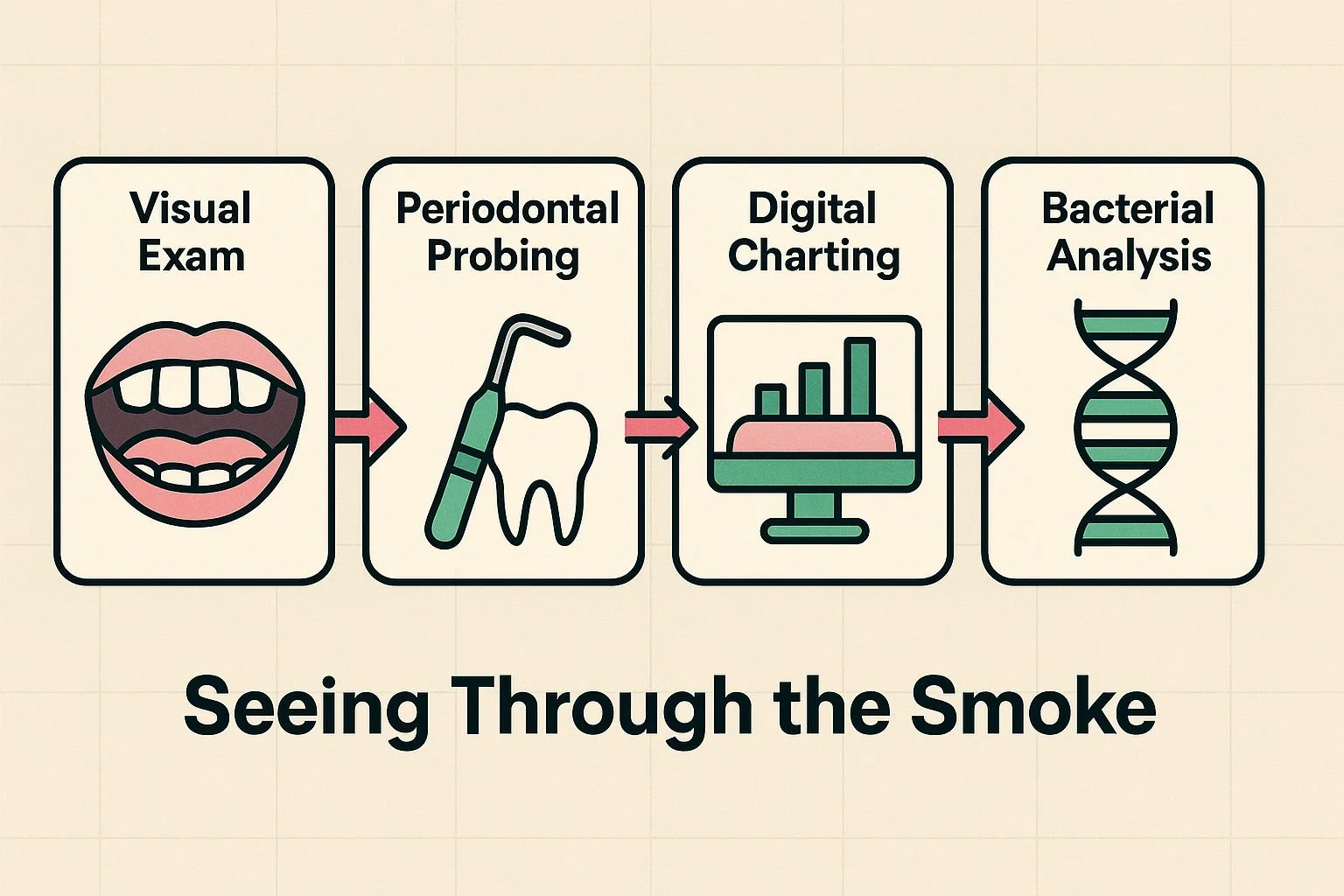
This infographic presents the diagnostic journey visualizing why traditional exams fail smokers and how advanced techniques uncover hidden gum disease.
Checklist: 5 Signs Your Gums Are in Trouble (Even Without Bleeding)
If you can't rely on bleeding to tell you when something is wrong, what should you look for? Watch out for these secondary signs:
Receding Gums: Your teeth are beginning to look "longer" than they used to.
Persistent Bad Breath: Nicotine thickens saliva, making it harder for your mouth to naturally wash away trapped bacteria and acids.
Changes in Your Bite: Your teeth feel slightly different when you close your jaw.
Dark Triangles: Small, dark spaces are opening up between your teeth near the gumline.
Tooth Mobility: You are noticing gum disease loose teeth—a major red flag that the supporting bone is degrading.
The Diagnostic Blind Spot: Why Traditional Exams Fail Smokers
Because of the nicotine-driven vasoconstriction, traditional visual dental exams can completely miss the early periodontal disease stages in smokers. A quick glance in the chair might result in a "looks good!" from a practitioner who is relying primarily on visual cues.
To truly see through the smoke screen, periodontal experts rely on a comprehensive diagnostic suite that doesn't depend on bleeding. At The Behrens Dental Practice in London, this diagnostic phase acts as a vital "Lie Detector Test" for gum health.
Instead of just looking at the surface, experts measure gum pockets—the hidden spaces between the tooth and gum where bone loss occurs. Through digital charting and advanced microbiological DNA analysis, practitioners can pinpoint exactly which specific strains of bacteria are active beneath the gums. This allows them to detect disease activity based on hard scientific data, completely bypassing the smoker's visual blind spot.
Beyond the Surface: Treating Advanced Presentation
Because the early warning signs are hidden, smokers very rarely catch their gum disease in its infancy. By the time they realize something is wrong—often because a tooth becomes loose or an abscess forms—they are already dealing with stage 3 gum disease or even advanced periodontitis.
Historically, the treatment for advanced gum disease involved highly invasive surgery: cutting the gums, folding them back to clean the roots, and stitching them up. For a smoker, this is a worst-case scenario. Remember that constricted blood flow? Healing requires robust blood flow. Surgical trauma in a smoker's mouth often leads to severe complications, intense pain, and failed healing.
This is exactly why modern, non-invasive technology has fundamentally changed the outlook for tobacco users.
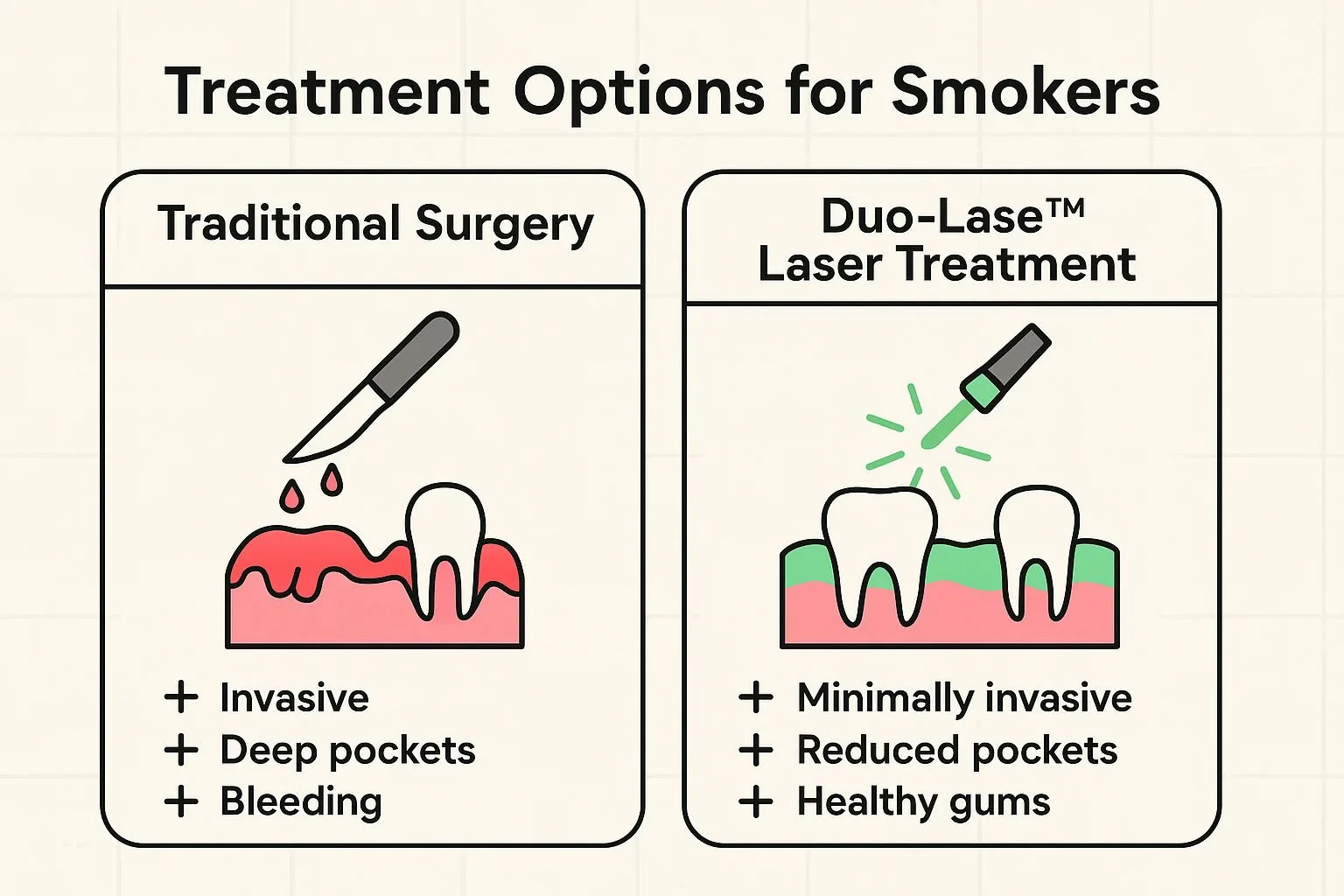
This comparison highlights Duo-Lase™ as a less traumatic, more effective laser treatment option tailored for smokers with advanced gum disease.
How Duo-Lase™ Bridges the Gap
Duolase is an innovative, non-invasive periodontal therapy exclusively offered at The Behrens Dental Practice. It is uniquely suited for the advanced cases that smokers frequently present with because it completely eliminates the need for cutting and sutures, thereby bypassing the compromised healing issues associated with smoking.
Unlike traditional methods, Duo-Lase™ utilizes a sophisticated dual-laser approach:
The Nd:YAG Laser (Photodynamic Pocket Decontamination): First, this highly specific laser targets and removes the dark-pigmented bacteria that cause the disease. It also acts as a powerful anti-inflammatory for the gum tissue, helping it heal. Crucially, it supports the creation of a brand new cell layer on the root surface—including cementoblasts (cells that form the hard tissue covering tooth roots)—which actively helps close the deep gum pockets.
The Diode Laser (Biostimulation): Second, a diode laser is applied. This step focuses on biostimulation, promoting further healing, triggering new collagen production in both the bone and the gum, and creating a natural fibrin seal to protect the pocket while it recovers.
Because there is no surgical trauma, patients require an average of 10 laser sessions (which can be completed up to 3 times per week). The procedure is so gentle that it is usually performed without any anesthetic, and there is zero downtime afterward.
The Smoker's Action Plan: Finding Stability
If you smoke, understanding that your body's alarm system is muted is half the battle. The next step is taking proactive control.
Seek Comprehensive Diagnostics: Do not settle for a quick visual check. Request full periodontal probing and ask about microbiological DNA testing to find out exactly what is happening beneath the gum line.
Commit to Quarterly Maintenance: Because your risk is higher and your symptoms are hidden, smokers require more frequent professional cleanings to maintain stability.
Explore Non-Invasive Options: If you have been told you need dental surgery or extractions, explore laser-assisted therapies that prioritize your body's ability to heal without trauma.
Frequently Asked Questions (FAQ)
Can you really have gum disease if your gums are pale and firm?
Yes. In smokers, nicotine constricts the blood vessels and causes gingival fibrosis (thickening of the gum tissue). Your gums may look pale and firm while the bone beneath them is actively being destroyed by bacteria.
Why don't my gums bleed when I smoke?
Nicotine restricts blood flow to the gum tissues. Without adequate blood flow, the natural inflammatory response—which causes the swelling and bleeding associated with early gum disease—cannot occur.
Does mouthwash help gum disease if I am a smoker?
While a good oral hygiene routine is essential, people often wonder, does mouthwash help gum disease? Mouthwash only tackles surface bacteria. It cannot penetrate the deep periodontal pockets where the disease-causing bacteria actually live and destroy bone.
Can hidden gum disease affect the rest of my body?
Absolutely. The bacteria trapped under your gums can enter your bloodstream. In fact, research shows that having advanced gum disease linked to heart disease diabetes stroke alzheimer’s is a significant clinical reality, making early detection even more critical.
Next Steps on Your Journey
Realizing that your symptoms may be masked by smoking can be an "aha moment" that completely changes how you view your oral health. You don't have to wait for a tooth to become loose to take action.
By utilizing advanced microbiological DNA analysis and dual-laser treatments that promote natural healing without surgical trauma, preserving your natural teeth is more achievable than ever before.